A Parent’s Guide to Standing
Answers to why children need to stand and how long to stand for maximum benefit





Your Physical Therapist has recommended you begin a standing program with your child, but you may be wondering why your child needs to initiate a standing program, and how it will help your child develop. If you are apprehensive about using a stander, hopefully this brochure will answer some of your questions and help you explain to family members the “Why” of standing

Medical Benefits of Standing
• Build overall core strength and head control
• Improve muscle memory and motor control to help your child learn to stand with less support
• Develop strength and endurance to stand longer time periods
• Standing may help build capacity to stand unsupported and take steps with assistance in the future
• Keep your child’s body healthy as they grow improved digestive health
For more information, click the button below.

“Standing helped my son Easton get stronger after his shunt revision and brain bleed.”
Lisa Johnson – parent of Easton (meningitis. CP)

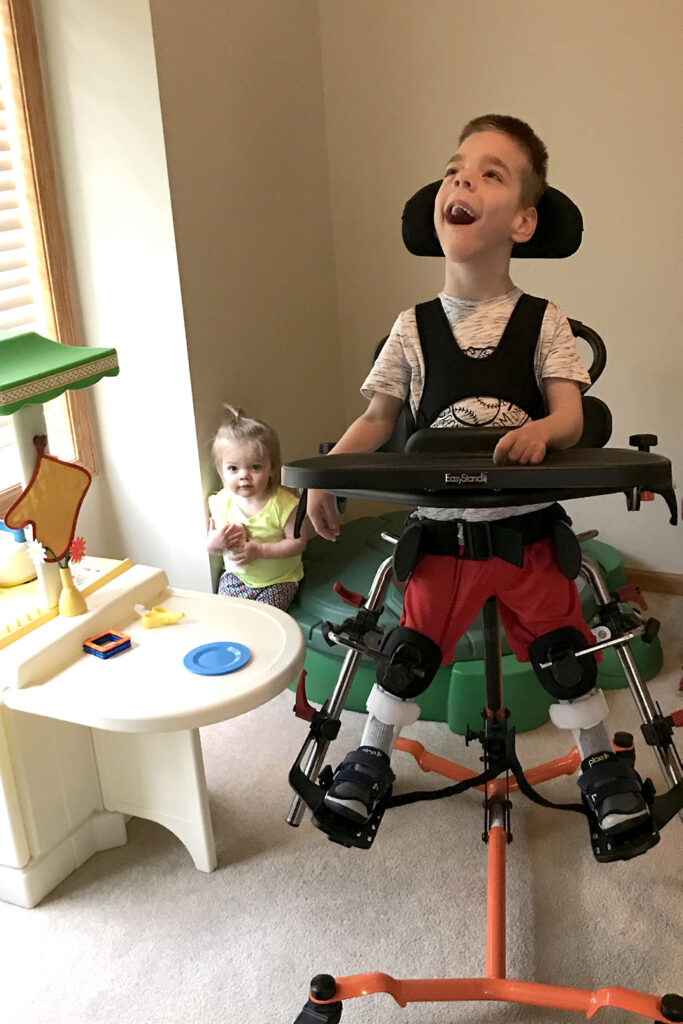
“We have been using a stander with RJ since he was one. Standing has helped him with his hip development, strengthening his whole body and keeping his GI moving -which makes everyone
Jess and Mike
happy!”
parents of RJ
(hydrocephalus, CP)
Bone Density
Children who participate in a standing program
can help reduce their chance of bone fractures by
building up the density of their bones. Research
shows standing at least 60 minutes daily is needed
to maintain good bone density for the prevention of
fractures. Standing for multiple episodes a day that
total up to 60 minutes is a beneficial way to gain
bone density benefits.
Range of Motion
Standing can help your child maintain their flexibility as they grow. If your child spends time in a special chair or wheelchair or is not able to move around as easily on their own; their muscles are susceptible to getting tight as they grow. Standing is one way to fit stretching into your child’s daily routine. Maintaining flexibility will make daily activities such as bathing, dressing, and getting into and out of a wheelchair easier as children grow. Research shows that children need to stand at least 45 minutes at one time to gain the benefits of improving or maintaining their muscle range of motion
Hip Integrity
Your child may be asked to stand in a stander that
allows hip abduction. if your child stands with
hips moved outward in a position of hip abduction
standing may help prevent secondary hip integrity
issues such as a hip subluxation or hip dislocation.
When standing with hips outward, children can
also, maintain hip flexibility; making daily cares
such as dressing, and bathing easier for parents.
Research shows children need to stand 45 minutes
a day with hips in 15-30 degrees of hip abduction to
maintain hip integrity
Hip Surveillance
In this section we will cover the benefits of a Hip Surveillance program for children with Cerebral Palsy or other disabilities. Hip socket development and associated complications for children that are unable to stand unsupported are increasingly being identified as areas of increased concern. One example is the increasing prevalence of Hip Surveillance programs. Standing, and more specifically, abducted standing, has been identified as one therapeutic intervention in some hip surveillance programs.
Why are Hip Surveillance programs being implemented?
One in three children with Cerebral Palsy (CP) will develop progressive hip dysplasia, which can affect their ability to sit, stand or ambulate, as well as cause pain. Early detection and intervention can minimize the need for later procedures or surgeries and improve quality of life. Children with GMFCS levels III-V appear at greatest risk. A child is at risk for hip displacement if he/she has cerebral palsy. Cerebral palsy affects a child’s ability to move. When children are late to stand and walk or can only do so with help, the hip joint may not develop as expected. In addition, the muscles that pull the legs together and up are often tight or stiff and can pull the hip out of place.






Why do we want to do Hip Surveillance?
• Children with cerebral palsy are more likely to have a hip problem called “hip dysplasia.”
• Hip dysplasia is when the thigh bone (femur) and the hip bone (pelvis) don’t grow into the right shape for the hip joint to work well.
• Hip dysplasia can lead to “hip dislocation” (where the thigh bone doesn’t stay tight against the bone of the pelvis anymore).
• Hip dislocation may be painful and may lead to problems with sitting, standing and changing clothes or diapers.
• Research has shown that children are more likely to get hip dysplasia if they are unable to move or stand.
• Researchers in Australia and Sweden have found that we can prevent hip dislocation by doing regular x-rays and hip exams and implementing other treatment accordingly.
Who is implementing these programs?
Some of the largest school districts in the United States, along with several international organizations that pioneered such programs, have established and implemented large-scale Hip Surveillance programs to screen young children with cerebral palsy on a regular basis and detect early-stage problems, with the goal of improving treatment strategies and outcomes.


Where are Hip Surveillance Programs being implemented?
Australia: https://ausacpdm.org.au/professionals/hip-surveillance/australian-hip-surveillance-guidelines/
Sweden: http://cpup.se/in-english/
United Kingdom: Spasticity in children and young people-Support for education and learning: practice-based implementation advice: NHS
- National Institute for Health and Clinical Excellence,
September 2012: https://www.nice.org.uk/guidance/CG145
Shriner Hospital for Children- N. California: www.hipscreen.org
Boston Children’s Hospital Orthopedic Center: bostonchildrens.org/cp
Zing standers provide premium features, support and comfort for children who are unable to stand unsupported. Regardless of diagnosis, whether its muscular dystrophy, cerebral palsy, spina bifida or others, a Zing standing frame can be configured with robust support wherever it is needed. Growth was a driving force behind the design of the Zing. Zing size 1 standers, in general, will fit most children as young as 9 months up to age 5. After age five, the Zing size 2 can fit kids from 32″ to 60″ while still providing all of the same features. These standers are not just top of the line because of support and comfort options, the entire Zing line features anatomically correct, independent leg abduction and are the only multi-position standers to perform true supine to prone in one motion.
Product Highlight




PK5010 Zing Portable
Fits kids up to 36″(91.5cm) and up to 36lbs(16.3kg)
Building upon the industry-leading innovation and features of the Zing multi-position stander, the new Zing Portable stander is a leap forward in product design. This new early intervention stander is the first “rightsized” product for standing children as young as possible (fits children from infancy to 36″ and up to 36 pounds). Typically developing children will usually begin the processes of learning to stand between 9-13 months. The Zing Portable is designed to fit this age group better than any other product available, but that is just one of a long list of features that creates a new standard of care.
For more information about the Zing Advantage and how Zing can help your child stand, click the button below.

Not sure what the next steps are? Check out our Funding Guide for information on getting a stander or Request a FREE Product Demo.
References:
Elkamil A, Andersen G, Hagglund G, et al. Prevalence of hip dislocation among children with cerebral palsy in regions with and without a surveillance programme: a cross sectional study in Sweden and Norway. Musculoskeletal Disorders 2011, 12:284.
Gordon GS, Simkiss DE. A systematic review of the evidence for hip surveillance in children with cerebral palsy. J Bone Joint. Surg Br. 2006 Nov; 88(11):1492-6.
Hägglund G, Alriksson-Schmidt A, Lauge-Pedersen H, et al. Prevention of dislocation of the hip in children with cerebral palsy: 20-year results of a population-based prevention programme. Bone Joint J. 2014 Nov; 96-B
(11):1546-52.
Hermanson M, Hagglund G, Riad J and Wagner P. Head-shaft angle is a risk factor for hip displacement in children with cerebral palsy. Acta Orthopaedica 2015, 86 (2): 229-232.
Kentish M, Wynter M, Snape N, Boyd R. Five-year outcome of state-wide hip surveillance of children and adolescents with cerebral palsy. J Pediatr Rehabil Med. 2011; 4(3):205-17.
Larnert P, Risto O, Hagglund G, Wagner P. Hip displacement in relation to age and gross motor function in children with cerebral palsy. J Child Orthop 2013, 8:129-134.
Murnaghan ML, Simpson P, Robin JG, et al. The cerebral palsy hip classification is reliable: an inter- and intra-observer reliability study. J Bone Joint Surg (Br) 2010, 92-B 436-41.
Robb JE, Hagglund G. Hip surveillance and management of the displaced hip in cerebral palsy. J Child Orthop 2013, 7:407-4138.
Shore B, Spence D, Graham H. The role for hip surveillance in children with cerebral palsy. Curr Rev Musculoskelet Med. 2012 Jun; 5(2):126-34.
Soo B, Howard JJ, Boyd RN, et al. Hip displacement in cerebral palsy. J Bone Joint Surg Am. 2006 Jan; 88(1):121-9.
Wynter M, Gibson N, Kentish M, et al. The Consensus Statement on Hip Surveillance for Children with Cerebral Palsy: Australian Standards of Care. J Pediatr Rehabil Med. 2011; 4(3):183-95.
Wynter M, Gibson N, Willoughby KL, et al. National Hip Surveillance Working Group. Australian hip surveillance guidelines for children with cerebral palsy:
5-year review. Dev Med Child Neurol. 2015 Sep;57(9):808-20.

